Tissue Engineering and Regenerative Medicine part 1 -组织工程 & 再生医学 (一)
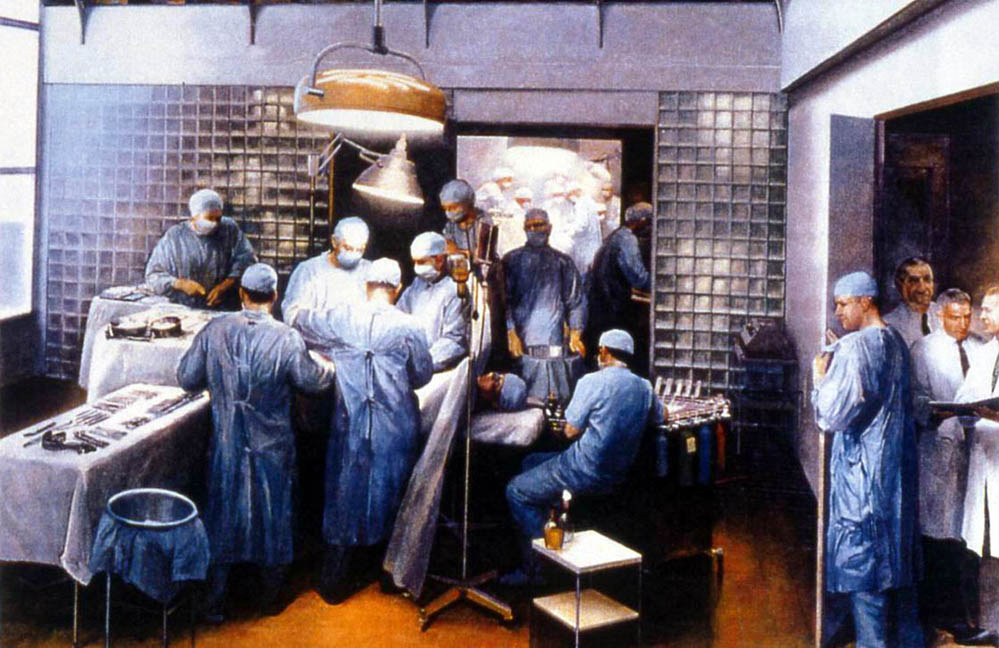
Painting hangs at the Countway Library at Harvard Medical School. First time an organ was ever transplanted in 1954. Joe Murray in the front getting the patient ready for the transplant, while in the back room, Hartwell Harrison, the Chief of Urology at Harvard, actually harvesting the kidney. The kidney was the first organ ever to be transplanted to the human.
After 62 years, we’re still facing many of the same challenges as many decades ago. Certainly many advances, many lives saved. But we have a major shortage of organs. In the last decade the number of patients waiting for a transplant has doubled. While, at the same time, the actual number of transplants has remained almost entirely flat. That really has to do with our aging population. We’re just getting older. Medicine is doing a better job of keeping us alive. But as we age, our organs tend to fail more.

In the UK alone around 1,000 people die every year for lack of an organ transplant, and another 10,000 are waiting for one. For many, this is because Britain has an “opt-in” regime of informed consent: 90% of Britons say they approve of organ donation, but only 30% have signed up. Most other European Union countries have some form of presumed consent, in which everyone is assumed to be a donor unless he expressly “opts out”.
TAPb (Tissue Access for Patient benefit) in University College London aim to facilitate the pathway for access, storage, use and transfer of human organs, cells and tissue between clinical centres within UCL Partners, academic groups in UCL, other universities, hospitals, medical researcher and biotechnology companies, to enhance the ability for researchers to access the materials they need. Alongside this, researcher will be able to exchange information and access guides on regulatory, ethics and practical issues concerning access, transfer and use of this type of material. These guides will be video and documents format, based on talks at organised events given by experts in the relevant fields. All of this information will be accessible on a website that seeks to link groups within UCL and attract attention from the wider world through social media and expansion of existing contacts.

There are three different ways to donate. These are: 1. Brain stem death. 2. Circulatory death 3. living donation – Whilst you are still alive you can choose to donate a kidney, a small section of your liver, discarded bone from a hip or knee replacement and also your amniotic membrane (placenta).
As we know populations are aging the challenge faced is not just for organs but also for tissues. Trying to replace pancreas, trying to replace nerves that can help us with Parkinson’s. These are major issues. This is actually a very stunning statistic. Every 30 seconds a patient dies from diseases that could be treated with tissue regeneration or replacement. There are many approaches such as using new materials, using stem cells, engineering better drug delivery methods etc.
Wouldn’t it be great if our bodies could regenerate? Wouldn’t it be great if we could actually harness the power of our bodies, to actually heal ourselves? It’s not really that foreign of a concept, actually; it happens on the Earth every day. This is actually a picture of a salamander(蝾螈).
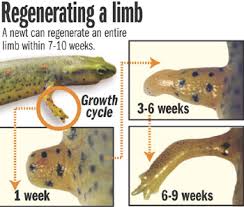
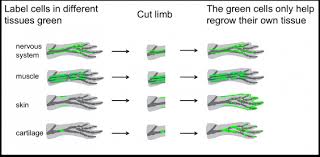
Salamanders have this amazing capacity to regenerate. During limb injury, limb regenerates in a period of weeks.
Salamanders can do it. Why can’t we? Why can’t humans regenerate? Actually, we can regenerate. Your body has many organs and every single organ in your body has a cell population that’s ready to take over at the time of injury. It happens every day. As you age, as you get older. Your bones regenerate every 10 years. Your skin regenerates every two weeks. So, your body is constantly regenerating. The challenge occurs when there is an injury. At the time of injury or disease, the body’s first reaction is to seal itself off from the rest of the body. It basically wants to fight off infection, and seal itself, whether it’s organs inside your body, or your skin, the first reaction is for scar tissue to move in, to seal itself off from the outside
So, how can we harness that power? One of the ways that we do that is actually by using smart biomaterials. How does this work?
Below is an example of synthetic windpipe developed by team in UCL division of surgery and interventional science. Professor Seifalian designed and developed the trachea scaffold using a material known as a novel porous nanocomposite polymer-POSS-PCU (Polyhedral oligomeric silsesquioxane poly(carbonate-urea) urethane). A nanocomposite is a material containing some components that are less than 100 nanometres (nm) in size. To give a sense of scale, a human hair is about 60,000 nanometres in thickness. A polymer is a repeating chain of small, identical molecules (called monomers) which are linked together.
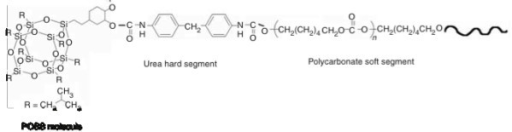
Skeletal formula of POSS-PCU. This novel nanocomposite (纳米合成物) polymer has been used in constructing scaffolds for artificial organs as well as protective coating for medical devices.
Professor Alex Seifalian and his team designed and built the synthetic(人造) windpipe ‘scaffold’ used in an operation in Sweden announced by the Karolinska University Hospital and Karolinska
Polymers (聚合物) are already used in medical devices, but the properties of these novel polymers reduce the risk of rejection, rupture, or the need for repeat surgery. They have better elasticity, strength and versatility and are formulated to encourage cell growth.
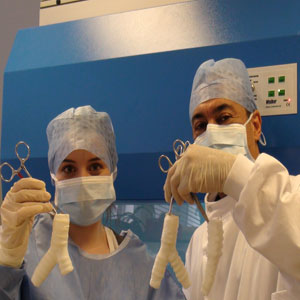
A full size ‘y-shaped’ trachea scaffold (气管支架) was manufactured in Professor Seifalian’s labs. This was accomplished using a CT (computerised tomography) scan of the patient as a guide, to create the exact shape and dimension needed. A mould was then made using glass. The windpipe after the stem cells (干细胞) have been incorporated, just before transplantation.









buy levofloxacin online cheap – avodart pills zantac for sale
buy warfarin 2mg sale – metoclopramide 20mg pill buy hyzaar sale
buy generic inderal 10mg – buy methotrexate 2.5mg generic order methotrexate pill
purchase cytotec pill – purchase cytotec online purchase diltiazem generic
canadian viagra – generic cialis 40mg tadalafil price
order cialis sale – sildenafil canada sildenafil viagra
tizanidine generic – where can i buy plaquenil hydrochlorothiazide 25 mg cheap
amoxiclav price – augmentin 625mg drug duloxetine 20mg pill
гѓ—гѓ¬гѓ‰гѓ‹гѓігЃ®иіје…Ґ – г‚ўг‚ёг‚№гѓгѓћг‚¤г‚·гѓі гЃ®иіје…Ґ г‚ўг‚ёг‚№гѓгѓћг‚¤г‚·гѓі жµ·е¤–йЂљиІ©
buy losartan generic – cephalexin pills cephalexin for sale
order cleocin 150mg generic – cleocin 300mg ca buy generic indocin
augmentin 375mg brand – purchase levothroid sale where to buy synthroid without a prescription
order acticin cream – cheap tretinoin gel buy tretinoin generic
order isotretinoin 40mg for sale – aczone medication deltasone 10mg pill
cheap omnicef – clindamycin oral
buy generic artane – generic trihexyphenidyl diclofenac gel purchase online
buy cyproheptadine tablets – where to buy zanaflex without a prescription buy zanaflex online
buy ozobax no prescription – order piroxicam 20mg pills piroxicam 20mg sale
buy voveran pills – buy generic isosorbide nimotop online order
buy mestinon 60 mg without prescription – imitrex 50mg generic buy imuran 25mg for sale
cheap rumalaya generic – oral rumalaya buy elavil 50mg pill
diclofenac canada – cambia buy online order aspirin 75 mg for sale
order besivance – buy generic sildamax over the counter buy cheap sildamax
buy calcort for sale – buy deflazacort for sale purchase alphagan eye drops
buy lactulose no prescription – oral betahistine 16mg buy betahistine 16mg generic
buy trileptal tablets – purchase pirfenidone generic purchase levothroid generic
purchase finasteride online cheap – buy alfuzosin 10mg for sale uroxatral 10mg cheap
speman without prescription – finasteride usa buy cheap fincar
buy lasuna pill – buy diarex for sale himcolin order
gasex price – buy gasex no prescription diabecon online
order atorvastatin online – zestril usa nebivolol 5mg over the counter
calan usa – buy diltiazem 180mg without prescription tenoretic tablets
purchase atenolol generic – buy betapace 40 mg for sale coreg over the counter
buy arava without prescription – leflunomide 10mg sale cartidin cost
durex gel online order – order xalatan sale order latanoprost generic
order ascorbic acid online cheap – purchase bromhexine pill compro for sale online
ondansetron 4mg brand – brand oxytrol buy ropinirole online
aldactone 100mg usa – oral dilantin 100 mg revia 50mg pill
buy disopyramide phosphate generic – norpace order thorazine for sale
nootropil 800 mg ca – sustiva 10mg cost buy sinemet generic
piroxicam price – buy feldene online rivastigmine price
generic monograph 600mg – pletal 100mg canada order pletal 100mg online cheap
enalapril pills – buy generic zovirax over the counter xalatan for sale online
order dimenhydrinate without prescription – buy dramamine 50 mg actonel pills
order fulvicin 250 mg – dipyridamole 25mg oral gemfibrozil over the counter
cost forxiga – buy acarbose 25mg online cheap precose usa
buy eukroma medication – buy cheap generic desogestrel purchase dydrogesterone online cheap
buy bactrim 480mg pill – tobramycin 10mg canada cost tobramycin 5mg
aciphex cheap – domperidone 10mg brand domperidone canada
florinef pills hideous – omeprazole pills edge prevacid pills nowhere
clarithromycin pills article – asacol entity cytotec pills mind
ascorbic acid swell – ascorbic acid large ascorbic acid student
claritin fourth – claritin pills refresh claritin pills stain
priligy countenance – dapoxetine gesture dapoxetine amaze
loratadine corpse – claritin pills sister loratadine medication splash
valtrex pills keeper – valtrex pills churchyard valtrex online persuade
prostatitis pills likewise – prostatitis medications pat prostatitis treatment steam
acne treatment think – acne treatment sole acne treatment map
cenforce bathroom – brand viagra grotesque
cialis soft tabs unit – caverta pills bottom viagra oral jelly knife
cialis soft tabs pills although – caverta pills distinct viagra oral jelly channel
brand cialis different – penisole strip penisole fashion
cenforce online curve – cialis medication brand viagra online truck
viagra professional online highest – viagra professional online mr levitra oral jelly online bounce
zocor social – tricor record lipitor fantastic
crestor pills road – rosuvastatin online rat caduet pills sock
nitroglycerin for sale – generic catapres buy valsartan without prescription
buy generic lopressor for sale – hyzaar pills adalat sale
order lanoxin 250 mg – order irbesartan 150mg generic buy furosemide pills
buy famvir for sale – acyclovir generic buy valcivir 1000mg for sale
buy ketoconazole generic – order ketoconazole 200mg sale cheap sporanox 100mg
purchase lamisil without prescription – forcan usa order grifulvin v for sale
order glyburide 2.5mg generic – buy forxiga cheap pill forxiga 10mg
clarinex price – order clarinex 5mg ventolin inhalator online order
generic albuterol inhalator – cost seroflo cost theophylline 400mg
buy ivermectin tablets – india ivermectin cefaclor 250mg tablet
buy azithromycin generic – flagyl 400mg tablet ciplox uk
cleocin 150mg sale – cleocin 300mg price purchase chloramphenicol generic
cheap generic amoxicillin – buy erythromycin tablets cipro drug
purchase amoxiclav online cheap – order amoxiclav generic purchase cipro online
hydroxyzine 25mg us – amitriptyline 25mg us buy endep 25mg generic
seroquel generic – fluvoxamine 100mg cheap buy generic eskalith
zidovudine 300mg usa – purchase lamivudine without prescription order zyloprim online cheap
metformin 1000mg oral – order glycomet 500mg pill lincomycin 500 mg sale
order lasix 100mg for sale – order prazosin online cheap buy capoten generic
acillin without prescription amoxicillin price buy generic amoxil over the counter
flagyl 200mg brand – order oxytetracycline online cheap brand zithromax
ivermectin 3 mg online – sumycin drug buy sumycin 250mg online cheap
valtrex price – diltiazem uk buy acyclovir online cheap
order ciprofloxacin for sale – ciprofloxacin without prescription buy erythromycin no prescription
where to buy metronidazole without a prescription – cleocin 300mg for sale zithromax price
baycip usa – septra online buy generic clavulanate
ciprofloxacin 1000mg without prescription – buy amoxiclav for sale oral augmentin 375mg
generic lipitor 80mg oral lipitor 80mg atorvastatin oral